 As a result, noninvasive pacing reemerged, in the 1980s, as a therapy for bradycardia and asystole. Transvenous pacing has served as the mainstay of urgent temporary pacing since then, although the significant time and operator skill needed to implement the technique are less than ideal. With the development of transvenous pacing leads later in the 1950s, interest in external pacing waned. However, the high current densities that the skin electrodes required to pace the cardiac tissue in those early devices caused painful stimulation of the cutaneous nerves and underlying skeletal muscles. Transcutaneous pacing was first introduced by Zoll and associates 1 in 1956 as a novel method of treating asystole and significant bradyarrhythmias. Adequate sedation and analgesia are essential in ensuring patient comfort. 
Proper skin preparation and electrode positioning ensure successful capture in most situations. The hemodynamic response to pacing also must be confirmed by assessing the patient’s arterial pulse. On electrocardiography, successful capture usually is characterized by a widened QRS complex, followed by a distinct ST segment and broad T wave. 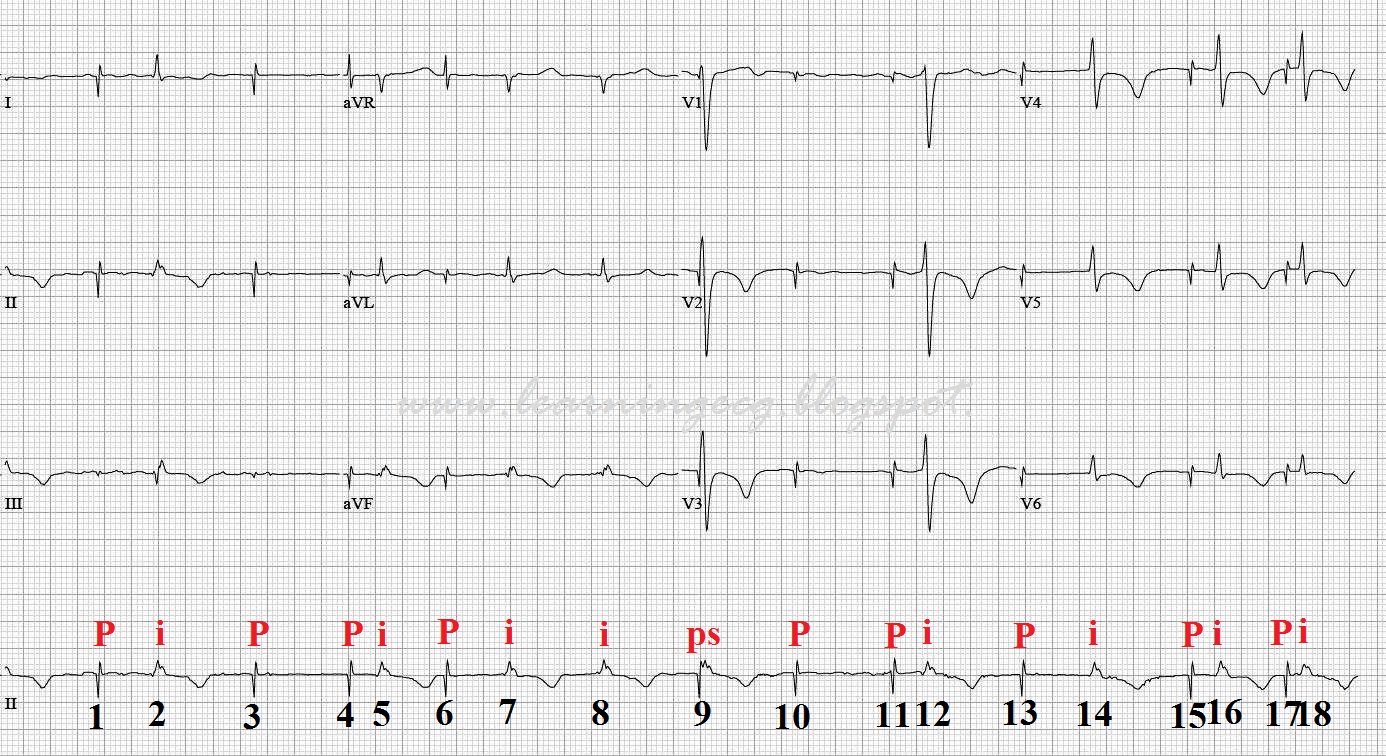
Most patients with minimal hemodynamic compromise require a current of 40 to 80 mA pacing thresholds tend to be higher in patients who have emphysema or pericardial effusion and in those who receive positive pressure ventilation. It is particularly helpful in patients with reversible or transient conditions, such as digoxin toxicity and atrioventricular block in the setting of inferior wall myocardial infarction, or when transvenous pacing is not immediately available or carries a high risk of complications. Transcutaneous cardiac pacing is a temporary method of pacing that may be indicated in patients with severe symptomatic or hemodynamically unstable bradyarrhythmias. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
